Follow Dr. Win Huang to Learn Clinical Thinking (Case 5) Severe Knee Pain in Osteoarthritis — But the Real Problem Wasn’t the Joint
Follow Dr. Win Huang to Learn Clinical Thinking (Case 5)
Severe Knee Pain in Osteoarthritis — But the Real Problem Wasn’t the Joint
This patient was a 68-year-old woman who came with her daughter. She had suffered from knee pain for many years, but in recent months her right knee had worsened significantly.
She described the pain not as dull soreness, but as a sharp, stabbing sensation. It became much worse with walking, weight-bearing, or prolonged standing. She could no longer squat. Walking was difficult, and she often had to hold onto objects or use a cane. Because she moved less, she gained weight, creating a vicious cycle.
Both knees showed mild swelling and some deformity. Imaging also revealed joint space narrowing. Faced with a patient like this, most clinicians would immediately diagnose knee osteoarthritis. To be honest, that was my initial impression as well.
But one sentence from the patient made me pause and think deeper.
She said,
“It feels like there’s a rope pulling inside.”
It sounded simple, but it carried a lot of meaning. She further described a pulling sensation extending from the lower posterior thigh to the upper lateral calf — like a deep line of tension passing through the knee.
That description didn’t fully match typical osteoarthritis. It made me reconsider the case from a different angle.
During the physical exam, my thinking continued to shift. With gentle passive movement, she did not have severe pain — which is somewhat inconsistent with advanced articular degeneration. However, knee flexion was clearly limited. She experienced sharp pain beyond a certain range, and the asymmetry compared to the left side was obvious. This explained why she couldn’t squat — it was pain-limited motion, not simply stiffness.
Next, I examined local tenderness carefully.
There was no obvious tenderness in the anterior knee. Points such as Xuehai, Liangqiu, and Dubi were not particularly sensitive, and the patellar tendon was not remarkable either.
But when I pressed the lateral popliteal groove, everything changed.
The tenderness there was striking. The patient could barely tolerate pressure, and the pain radiated deep into the knee. Comparing both sides, the left knee had almost no tenderness. The asymmetry was very clear.
At this moment, my attention shifted — from the joint itself to the lateral popliteal groove as a structural region.
Anatomically, this area is a convergence zone where fascia, tendons, and neural pathways intersect. A new possibility immediately came to mind: this might not be purely a joint problem. Neural involvement could be present.
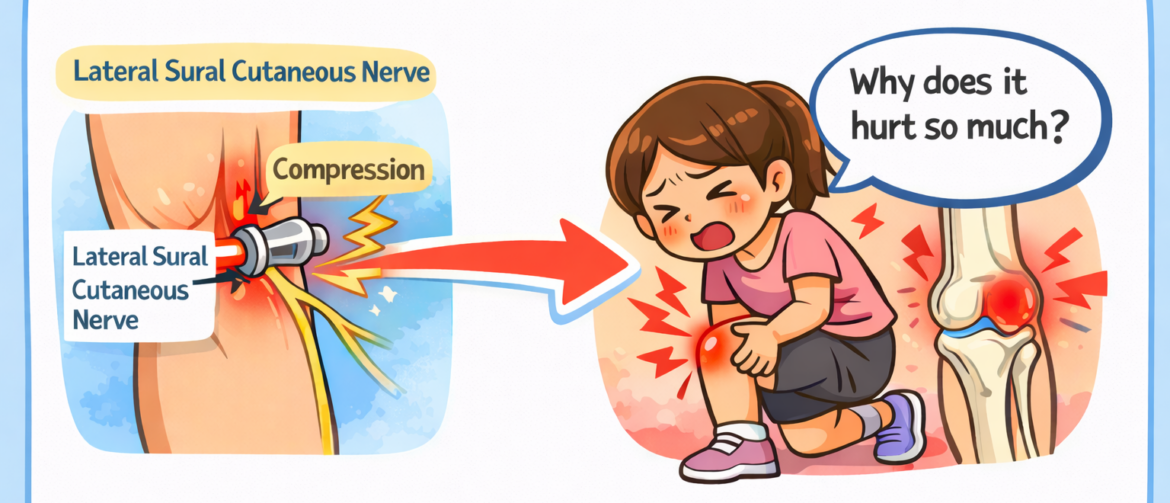
To confirm this, I examined sensation along the lateral aspect of the right lower leg. The result was clear — hypersensitivity in the upper lateral calf compared to the left side. This finding suggested involvement of the lateral sural cutaneous nerve.
In other words, this was not just joint pain. It was a structural problem with neural pathway involvement.
Functionally, chronic fascial tension in the lateral popliteal groove can lead to two consequences.
First, increased local fascial tension may restrict deep structures such as the popliteus muscle.
Second, compression of superficial sensory nerves passing through the region can produce referred sharp pain.
Suddenly, her symptoms made sense.
Why the pain was sharp.
Why it felt like a pulling line.
Why passive movement wasn’t severely painful.
Why weight-bearing aggravated it so much.
Once the thinking became clear, the treatment direction became obvious.
Instead of focusing solely on osteoarthritis, I targeted the fascial tunnel of the lateral popliteal groove.
I used three-edged needle pricking with mild bloodletting, followed by localized cupping, aiming to release fascial tension in this region.
The result was immediate.
The stabbing pain decreased significantly. Range of motion improved. Walking became easier, and she no longer needed to hold onto walls. The sharp pain that had troubled her for months nearly disappeared. She was genuinely happy, because she had never experienced such improvement from previous treatments.
It’s not surprising that she had been treated as a typical osteoarthritis patient elsewhere. The imaging findings supported it. Her age matched. Both knees showed swelling and deformity. Without deeper questioning and more detailed examination, it would be easy to remain trapped in this “reasonable diagnosis.”
But once the fascial compression in the lateral popliteal groove was released, neural irritation decreased and function improved immediately. This indicated that we had addressed the primary driver of symptoms, rather than being misled by background pathology.
This case gave me a very direct lesson.
In clinical practice, we often chase new techniques, new methods, and new schools of thought. But over time, you realize something important:
Rather than endlessly accumulating techniques, it is more valuable to refine one core ability — clinical reasoning.
Because when the diagnostic level is correct, treatment naturally gains direction.
And when the direction is correct, even simple interventions can produce powerful results.
 中文微信:nzacupunctureclinic
中文微信:nzacupunctureclinic
Leave a reply