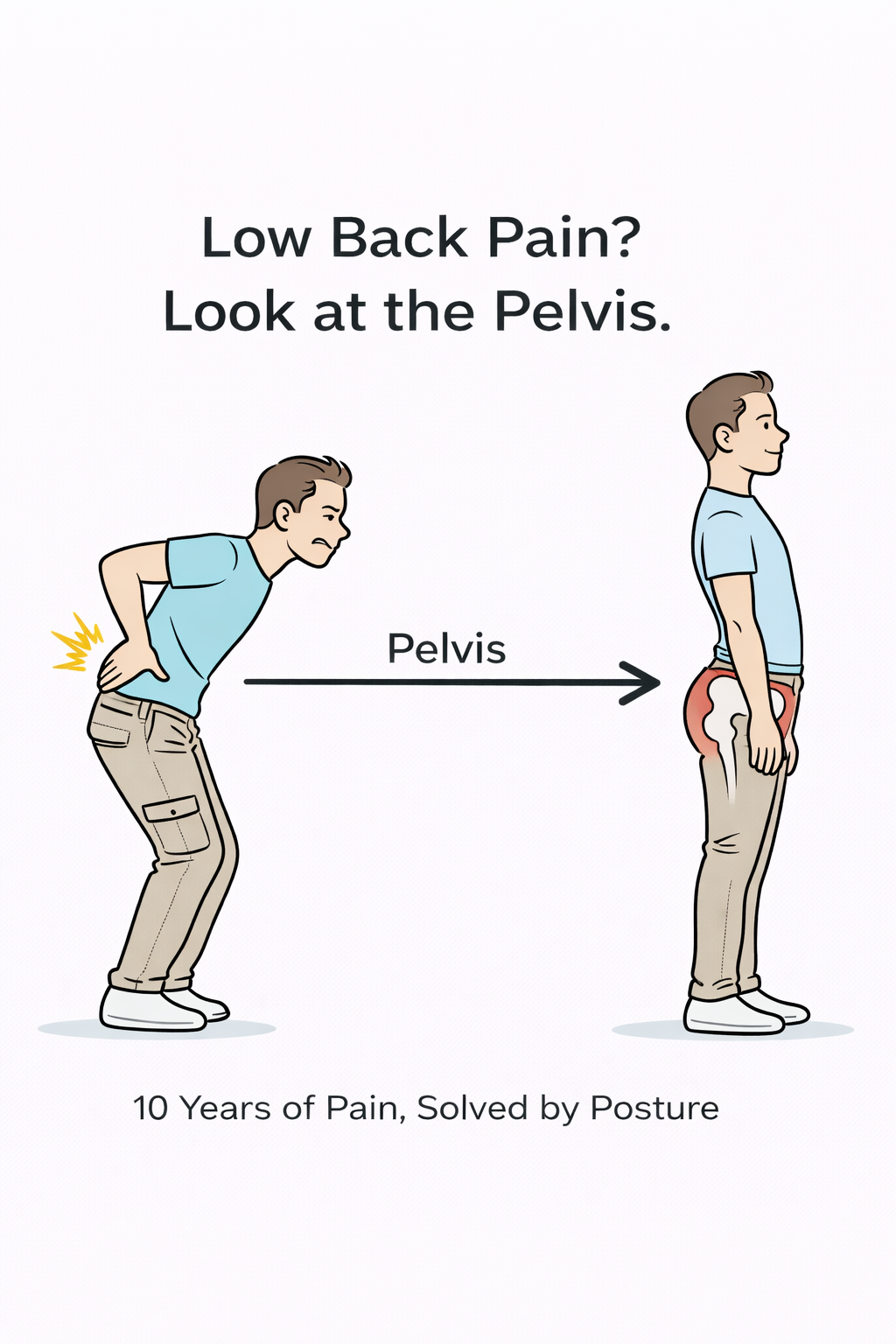
Following Dr. Huang in Clinical Practice (4)—A 10-Year Chronic Low Back Pain: The Answer Was Not at the Pain Site, but in the Posture
Following Dr. Huang in Clinical Practice (4)
A 10-Year Chronic Low Back Pain: The Answer Was Not at the Pain Site, but in the Posture
Some conditions are not hard to treat — they are simply misread for years.
This case was a classic example of clinical reasoning correction for me. I went through layers — muscles, fascia, joints — and finally stopped at the most easily overlooked level: posture.
The patient was a man in his mid-40s with more than ten years of chronic low back pain. Over the years, he had tried physiotherapy, chiropractic care, acupuncture, and massage. Every treatment helped a little, but nothing truly changed. The pain was almost constant — a dull ache around 6–7/10, occasionally reaching 8/10. The most distressing part was severe morning stiffness, and he could not lie flat to sleep. Forward bending was markedly limited; he could only reach just below the knees, far from touching his feet.
This type of patient is very common in clinical practice — the classic “treated everywhere but never truly better” group.
At the first visit, my thinking was fairly conventional. I assessed the likely pain generators and treated accordingly. Muscles showed no clear tender points. Nerve patterns did not resemble superior cluneal neuralgia. The sacroiliac joint was not strongly positive. It was not clearly muscular, neural, or articular. So I arrived at a common conclusion: chronic thoracolumbar fascia inflammation. I used floating needle therapy targeting the fascia. After the first treatment, the patient reported noticeable change and even said, “I think you got it right.” Many clinicians would stop here — once there is a response, self-confirmation comes easily.
But the improvement did not last. By the second and third sessions, progress plateaued. That made me reconsider. If this were purely fascial inflammation, it should not be this stubborn.
On the fourth visit, I re-examined him. This time, forward flexion provoked more pain around the sacroiliac region. There was mild but definite tenderness. My thinking shifted toward chronic sacroiliac joint dysfunction. I adjusted the treatment focus and performed local bloodletting and cupping. Again, some improvement — but still not the kind of release I was expecting.
When a chronic condition keeps shifting direction without truly resolving, you begin to sense that you are still missing the right level.
For a brief period, I even considered ankylosing spondylitis. Ten-year history, prominent morning stiffness, severe limitation in forward flexion — all red flags. I advised imaging and blood tests to rule it out. But two things did not quite fit: the pain pattern was not classically inflammatory, and flexibility consistently improved after treatment. That suggested a mechanical component rather than an autoimmune process.
The real turning point came during a very ordinary fifth visit.
The moment he took off his shirt, my first instinctive thought was: why is his abdomen projecting so far forward? This was not a logical deduction — it was a postural intuition. Many breakthroughs in clinic do not come from complex reasoning, but from simply looking again.
I asked him to stand sideways. The posture was obvious: anterior abdominal protrusion, glutes drifting backward, and an exaggerated lumbar lordosis. Then I had him stand against the wall. A classic sign appeared — the gap between his lower back and the wall was unusually large. When bending forward, the lumbar curvature persisted, flexibility was poor, and compensatory patterns were evident.
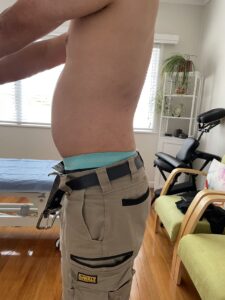
At that moment, the puzzle suddenly closed — he had anterior pelvic tilt.
If someone lives long-term in anterior pelvic tilt, what happens? The iliopsoas shortens chronically, the erector spinae remain overactive, while the glutes and hamstrings weaken. The lumbar spine stays in a high-load hyperlordotic state, and the posterior fascial chain is continuously under tension. Over time, all of this collapses into a simple complaint: low back pain.
Looking back at the earlier treatment stages became quite interesting. The fascia diagnosis was not wrong — chronic tension inevitably affects fascia. The sacroiliac reasoning was also not wrong — pelvic imbalance leads to SI compensation. But both were downstream findings. They were consequences, not the origin. We had been treating layers — superficial, intermediate, compensatory — without touching the true mechanical starting point.
This is the biggest trap in cases like this. Every step seems reasonable, yet none reaches the root.
This case reaffirmed something important for me: many chronic pain conditions are not isolated diseases, but the result of long-standing postural patterns. Especially in patients with long histories, recurrent treatments without resolution, pronounced morning stiffness, and limited forward flexion, we must ask a simple question — is this fundamentally structural?
When you encounter a decade-long low back pain that keeps recurring despite treatment, accompanied by morning stiffness, limited flexion, and anterior abdominal projection while standing, it is time to step out of local thinking. Do three simple things: observe the lateral posture, assess pelvic tilt, and perform a wall-gap test for lumbar curvature. Very often, you will discover that the real answer is not located at the pain site, but in the posture itself.
What this case ultimately gave me was not only a diagnostic correction, but a reminder about thinking. Clinical medicine is not just about locating pain — it is about understanding structural relationships. Sometimes the real cause is not hidden deep inside. It has been standing right in front of you all along.
 中文微信:nzacupunctureclinic
中文微信:nzacupunctureclinic
Leave a reply