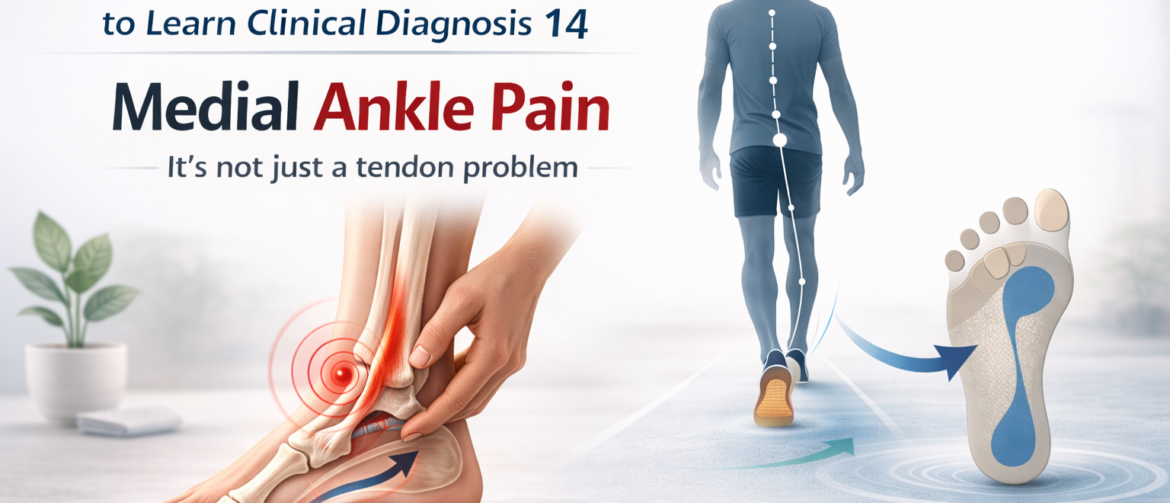
Follow Dr Win Huang to Learn Clinical Diagnosis (Case 14) Only After the Medial Ankle Pain Was Gone Did I Truly Start Treating the Patient
Follow Dr Win Huang to Learn Clinical Diagnosis (Case 14)
Only After the Medial Ankle Pain Was Gone Did I Truly Start Treating the Patient
This patient is a young male and also a returning patient of mine. This time, he came in with pain on the medial side of his right ankle.
The pain was not severe, but it had a very typical feature — pain with the first step in the morning. Each day when he got out of bed and put his foot on the ground, he would feel clear discomfort around the medial ankle. However, after walking a bit and warming up, the discomfort would reduce. During normal walking, he felt almost nothing, but once the activity level increased, such as playing basketball or football, the pain would gradually return.
He had a history of an ankle sprain several years ago, but this current pain had developed gradually over the past two to three months.
During examination, I palpated a relatively thick and tight “tendon-like structure” just anterior and inferior to the medial malleolus. Following this structure, it connected to a prominent, hard bony point. Pressing on the tendon produced a dull aching sensation, while pressing on the bony prominence caused more distinct pain.
My initial impression was straightforward — a local tendon inflammation.
So I treated it accordingly: local acupuncture with a small amount of bleeding technique. After two sessions, the pain was almost completely gone.
At that point, the case could have been considered “finished.” But I checked again. The tendon was still tight, and the bony prominence was still there.
At that moment, I knew clearly — the problem was not finished. The pain had been resolved, but the condition had not.
I then asked him to stand and deliberately change his weight-bearing pattern. When he shifted his weight slightly toward the lateral side of the foot, discomfort appeared again in the medial ankle.
This was the point where I moved beyond looking at a “single point.”
It told me that this was not just a local inflammation, but a problem of load distribution.
I reviewed the anatomical structure again. The prominent bone was the navicular, and the tight “tendon” was the posterior tibial tendon.
If I stopped here and simply called it “posterior tibial tendinitis,” it would still be insufficient. Because a simple tendon inflammation does not fully explain why the navicular is involved, nor why the symptoms change immediately with altered loading.
So I went one level deeper.
The posterior tibialis originates from the deep medial aspect of the tibia, runs behind the medial malleolus, and inserts into the navicular. It is a key structure in the medial support system of the foot. Its function includes maintaining the arch, controlling inversion, and resisting pronation.
Once this chain is under abnormal load for a long period, the posterior tibialis is forced to work continuously. Over time, the tendon becomes tight and thickened, and repeated traction at its insertion leads to stress at the navicular.
This is why we see a tight tendon and a prominent bone.
At this point, the mechanism of the case became clear.
It was no longer a problem at a “point,” but a state of overload along a “chain.”
Once the thinking reached this level, the treatment focus changed completely. It shifted from doctor-led local treatment to the patient relearning how to use his foot.
I gave him several simple exercises. First, heel standing to activate the anterior muscle group and reduce the constant pull on the medial side. Second, gently lifting the medial arch — not by force, but allowing the arch to “rise naturally,” redistributing support from the posterior tibialis to the entire plantar control system. Third, a light outward push exercise to engage the lateral muscles, sharing the load that was previously concentrated on the medial side. Finally, a very gentle stretch — with the foot slightly outward and the body leaning forward, to give some release to the overworked posterior tibialis. I specifically reminded him that the stretch should be light and relaxed, not forceful.
At this stage, the real treatment had just begun.
Because the disappearance of pain only means the alarm has been turned off. Rebalancing the load is what actually restores the system.
Many cases of medial ankle or navicular pain respond well to local treatment, but they also tend to recur. However, once you move from “point” to “chain,” and further to “system,” some problems can be stopped before they fully develop.
For me, the real value of this case was not that the pain was relieved, but that it reminded me not to be satisfied with simply “removing pain.”
 中文微信:nzacupunctureclinic
中文微信:nzacupunctureclinic
Leave a reply