
【E-book】 The Collection of PhD Win Huang Difficult Medical Cases
1, Left arm and hand pain and tingling | hand muscle lost | arm muscle lost | arm and hand weakness | Auckland acupuncture clinic
Please make an appointment, click below link
Left arm and hand pain and tingling | hand muscle lost | arm muscle lost | arm and hand weakness
left arm and hand tingling for 1 and half year, can not sleep due to the pain, take more painkillers, still stopping the pain, did 4 MRI, nothing find. did some treatments, no more improvement. two sessions of acupuncture, he feels good, pain relieving lots, sleep is good, no more tablets, keeping acupuncture.
my check finding was, that the left hand and arm muscles were lost, the left hand and arm felt dull, and the left tendon reflex was lower.
what do you think?
what kind of problem?
where is the nerve damage?
Thanks
My opinions:
we will think it is a nerve injury when you meet the patient who has tingling in the left arm and hand and lost muscle in the hand.
which some parts of the nerves of the arm and hand get injured, whether is an injury center of the nerve system or peripheral nerves?
the answer should be peripheral nerves because of the lost muscle in the hand.
so we will locate the damaged area, whether it is in the spine cord, the root of the nerves, the brachialis plexus, or the nerves in the upper limb.
from my check, the dull feeling is in the entire left arm, it is a normal feeling in the left chest and neck, so we know the nerve damage is in the C5- T1, it is almost impossible to get lesions in the cervical spine cord and nerves roots, and the reflex disappears, we can confirm it is not the cervical spine cord lesions, it is rare to get the injury only in the roots of C5-T1, and no the C4, and T2.
we know we will think of the brachialis plexus lesions if there are over two nerve injuries in the upper limb, the patient has numbness in the ulnar side of the left hand, triceps loss, and great thenar loss. it indicates he has radial, ulnar, and median nerve injuries, so we think it is the brachialis plexus lesions.
the patient did 4 MRI examinations on the neck, shoulder, back, and arm, and nothing was found, so we do not think it is the cervical vertebrae problem and tumor.
then we will be sure of the location of the lesion, generally, There are three easy nerve entrapment points, which are the scalene muscle point, supraclavicular fossa point, and pectoralis minor point.

the scalene muscle point is in the middle of the sternocleidomastoid muscle posterior edge, with more tenderness in the point, and the radiates pain to the arm and hand when I press the point, so he suffered from the brachial plexus entrapment ( scalene muscle point), and it mainly is the entrapment of the superior stem of the brachial plexus, because his motor weakness mainly is in the left hand.
in TCM, we think it is a “Wei syndrome”, because he has muscle loss in his left arm and hand and left arm and hand weakness, so it belongs to the “qi and blood deficiency, Malnutrition of meridians”, then we will choose the YANG MING meridians points, such as Hegu, Waiguan, Shousanli, and Jianyu.
because he has severe tingling in the left arm, so I think that his deficiency and Malnutrition are due to the entrapment of meridians. I will choose “the activates meridians method”, except I use the Yang-ming points, I will use the bloodletting cupping in the “Tianchuang point”
the patient feels much better, with no more pain at night, so sleep is very well, the power of the fingers is better too after two sessions of the bloodletting cupping in the “Tianchuang point”
keeping my treatments, I will tell you the result after 6 sessions of treatments.
Thanks reading!
2, Shoulder pain half year | tenderness radiates to arm and shoulder | one point one needle fast effect
Please schedule an appointment by clicking the link below:
A shoulder injury, X-ray and Ultrasound showed tear in shoulder tendon, still sharp pain in the shoulder, arm and back, no sleep due to the pain, what do you think this situation? Please let us know your opinion! I will put another video, lets you know what my thoughts . Thanks
My Opinion
Think of the shoulder sprained when we meet a shoulder sharp pain which is due to the gym and ultrasound report is a tear in the top of the shoulder but you maybe change your opinion after my physical examination and my treatment。
How to think of the shoulder pain? how to think of the ultrasounds report? for acupuncturist doing in general acupuncture , can we improved a shoulder pain completely?
today I will talk about the my opinion. at first, one shoulder pain for half year, more worse and worse , specially more pain at night, so we need change the diagnosis, maybe the pain come from the neck, maybe it’s the nerve blocked, from my check his feeling is dull and radiated sharp pain in the upper arm , so we know its a neuralgia.
second, the ultrasound report that the tear maybe be the old injury, maybe it is the reason of the shoulder pain in the early stage, but it isn’t a reason of the sharp pain at moment.
third, the general acupuncture is not stronger, we should choose specific point and specific needle, then it is immediately more effective.
3, shoulder nerve pain | frozen shoulder | hand color change | Thoracic outlet syndrome
Please schedule an appointment by clicking the link below:
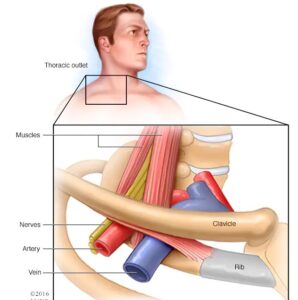
He is a patient who I met today, it is a very interesting medical case. He comes to see me for his frozen shoulder, his shoulder pain started from end of January, he could not move his left shoulder due to a sharp pain, he went to the physiotherapist who thought it was a frozen shoulder, did ultrasound, X-ray, and saw a specialist who did steroids injection, not much improvement. His friend recommended me to him, he wants to do acupuncture. When I asked his case history, he tells me his hand color changed when his shoulder had severe pain, so I don’t think his shoulder pain is only frozen shoulder, then I did a neurological examination for him.
I found his left arm reflex is lower than right,
Left arm feels dull,
Muscle power is normal,
More Tenderness in the point under collarbone and the pain radiates down to left arm,
So I think it is a Thoracic outlet syndrome (the point between collarbone and first rib)
His shoulder pain is neuralgia, his [frozen shoulder] is due to the severe pain, and frozen shoulder is the second symptom.
what do you think ?
Thanks
My opinions
1, How should a therapist think of the case when you meet a patient who says he has a frozen shoulder, shoulder pain, limited movement of the shoulder, Ultrasound report was a inflammation and tendon swelling, the specialist did steroid injection, and the patient has done physiotherapy for his frozen shoulder. I mean it is a frozen shoulder from every evident. I dare say that we will do treatments based on frozen shoulder over 95% therapists.
2, We will get the same results like these therapists who did physiotherapy and injection if we will do treatments for his frozen shoulder. It will get worse and worse, because it is not real frozen shoulder. I do know the fact that it is not real frozen shoulder as his hand has color changes and has numbness in the left arm when he has a severe shoulder pain.
3, We know it is a neuralgia from brachial plexus injury, because we found his arm feels dull, reflex is lower, and the Tinel’s sign positive. in generally, there are three injury points for a brachial plexus injury. They are, scalene muscle point, the point between collarbone with first rib, and pectoralis minor point. There is a more tender point under the left collarbone, and the tenderness radiates to the left arm, so it is a Thoracic outlet syndrome (the point between collarbone and first rib) for this case.
4, Why do I think it is not real frozen shoulder? First, his hand color changes when he have a severe shoulder pain; Second, there was not good results after physiotherapy and injection, and it got worse and worse.
5, Especially for difficult cases, we will get some important information from case history and physical examination. Then carefully ask patient, and do every kind of test. Then get a correct diagnosis, and do the correct treatment.
6, I have discussed with the patient. At the moment we do two steps at the same time, one way is doing acupuncture, another way, he will see a neurological specialist and do CT scans in neck and chest.
4, pain in the right hamstring and knee| walk with a limp| sciatica | common peroneal nerve injury | Auckland acupuncture clinic
Yesterday I met a patient who told me that he suffered from sciatica for 3 weeks. he was walking with a limp to my consult room. He went to see a doctor and took painkillers, and then he went to see a physiotherapist, There was no more improvement, and his family doctor recommended a specialist to him, and he will do a lumbar MRI.
Short video for the people cannot watch the You tube.
What do you do in this situation for the patient, his doctor and physiotherapist did treatments, but he still has more pain in the leg and walks with a limp, and a specialist suggested he will do a Lumbar MRI. maybe many acupuncturists will do acupuncture based on sciatica with a lumbar problem, putting needles in the lower back, and leg.
For me, I will do a physical examination, especially a neurological exam, regardless of what the family doctor or specialist thinks. I will get my diagnosis in Western medicine through my exam and symptoms. I found these positive signs, dorsiflexion of the right foot is weakness, and dull feeling in the superior lateral of the right lower leg, so I do not think it is a lumbar spine, lumbosacral plexus problem, or sciatica.
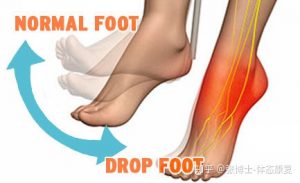
There rarely is a dropped foot if it is a lumbar spine disc problem, because it is a solo nerve root injury; not only they have the weakness of the dorsiflexion of the foot, but they also have the weakness of the plantar flexion of the foot if it is lumbar spine disc or lumbosacral plexus injury. In this case, it has only the weakness of the dorsiflexion of the right foot. so I think it is a common peroneal nerve injury.
For the common peroneal nerve entrapment, there are two types of entrapments, one is in the peroneal tube, which is very common in the clinical, another one is in the Popliteal fossa lateral groove.
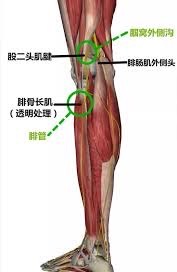 Lateral groove and peroneal tube
Lateral groove and peroneal tube
It does not have the hypoalgesia in the superior lateral of the right lower leg if the common peroneal nerve entrapment level is in the peroneal tube, for this case, I will not think it is a common peroneal nerve entrapment because there is a hypoalgesia superior lateral of the right lower leg.

the sensation of the superior lateral of the right lower leg is controlled by the Lateral sural cutaneous nerve which is divided from the common peroneal never over the peroneal tube. for this case, it has lateral sural cutaneous never injury and the common peroneal never injury, so the level of never entrapment is over the peroneal tube.

So, I think the entrapment level is in the popliteal fossa lateral groove, for this case, there is more tenderness in the area when I did the pressure. and the patient felt very well after the first session needle nerve relaxation method.
What do you think? hope to get your opinions!
5, lower back pain 7 months | 4 injections and one waiting injection | severe sharp lower back pain
Please schedule an appointment by clicking the link below:
He has had lower back pain for 7 months, he had an MRI which shows the root of the nerve L5L4 is damaged by the disc. He did 4 sessions of steroid injection and one waiting injection, but he still more sharper pain in both lower back, and the pain radiates down to both hamstrings, with no pain in both lower legs. a little bit of weakness in the lower back. He doesn’t want to do the 5th injection, his friend recommended me to him, try acupuncture.
A short video for could not watch YouTube
My opinions
1, What do we think about MRI results?
MRI shows left lumbar spine L4L5 disc Hernia, there are pain in the left lower back and leg, numbness in the left lower leg, and weakness in the left leg if it is a disc hernia, but for the case, lower back pain in both side, radiates to both thighs, he does not feel the left lower leg pain and numbness. I can not think it is a lumbar spine disc hernia. for example, if only a headache, let the patient do an MRI of the lumbar spine, we think the headache is due to the lumbar spine disc hernia if the MRI shows L5L4disc hernia. in the clinical, we can see many patients who do not feel symptoms, but the MRI shows a lumbar spine disc hernia.
2, Why don’t the practitioners do a general physical exam?
I will do a physical examination, especially the neurological exam. In this case, I found that the knee-tendon reflex is normal, and the straight leg raise test negative, but the areas of L1-L2, S3-S4 are not sharper. these examinations do not support the diagnosis of the lumbar disc hernia. why his practitioners do not do physical examinations?
3, What did I think of it from my general neurological examination?
there is only damage to the 3 cutaneous nerves ( superior gluteal cutaneous nerve, middle gluteal cutaneous nerve, Inferior gluteal cutaneous nerve, and femoral nerve cutaneous branch)from examination, he fell on the land, sprained the lower back muscle, muscle spasm damage the cutaneous nerves, the sharp pain in the lower back, 4 steroid injections are in the deep of lower back for the root of nerves, so the injections are unuseful.
4, what kind of ways is the acupuncture?
He had acupuncture twice, and 95% of the pain disappeared. His waist felt stronger and he walked normally. If it is a lumbar disc herniation, acupuncture should be ineffective, and even 4 injections of steroids show no improvement. So I thought it was a muscle injury, and then the cutaneous nerve was compressed. Acupuncture relaxes the muscles and then relaxes the compressed nerves, so the back pain disappears.
Medical Disclaimer
The medical information on any/all of our content is provided as an information resource only, and is not to be used or relied on for any diagnostic or treatment purposes. This information does not create any patient-physician relationship, and should not be used as a substitute for professional diagnosis and treatment. Please consult your health care provider before making any health care decisions or for guidance about a specific medical condition.
 中文微信:nzacupunctureclinic
中文微信:nzacupunctureclinic
Leave a reply