Follow Dr. Win Huang to Learn Clinical Medicine 6 . When Shoulder Pain Is Misled by Tender Points — The Answer Lies Deep in the Axilla
Follow Dr. Win Huang to Learn Clinical Medicine 6
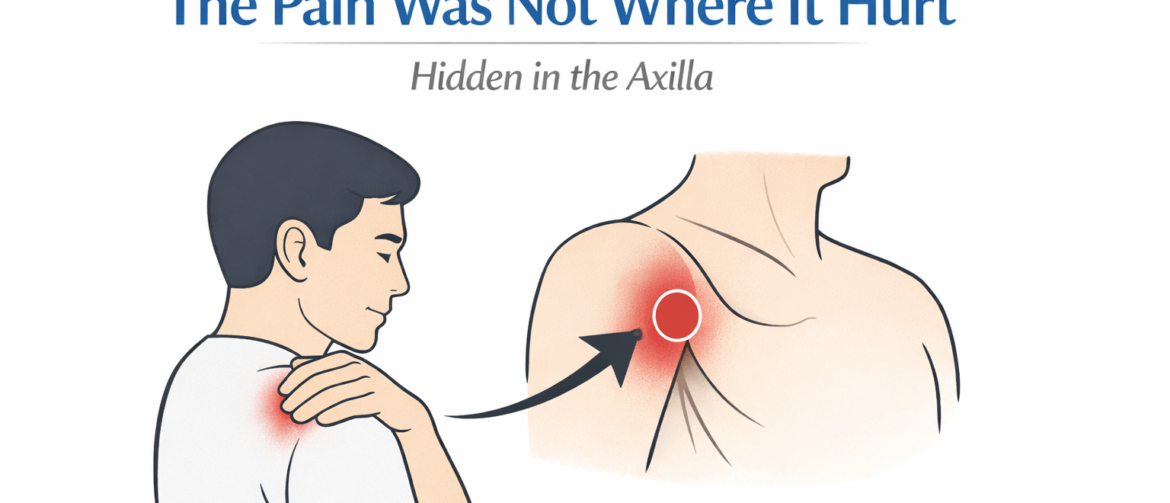
When Shoulder Pain Is Misled by Tender Points — The Answer Lies Deep in the Axilla
This patient is one of my long-time patients.
He had been experiencing right anterior shoulder pain for about three months.
Most of the time it didn’t hurt much, but certain movements would suddenly “ignite” the pain — especially reaching the arm backward, or lifting the arm up and pressing it downward. When sleeping, he could rest his head on his left arm, but doing the same on the right side was simply impossible.
Because of the pain, he had stopped exercising and decided to seek treatment.
The first examination: nothing obvious
On examination, there was almost no tenderness in either the anterior or posterior shoulder.
The bicipital groove was also non-tender, which made biceps long head tendinopathy unlikely. There were no signs pointing strongly toward classic impingement or obvious bursitis.
I asked him to localize the pain more precisely. He pointed to an area around the junction of the upper and middle third of the humerus, near the anterior border of the deltoid. Yet interestingly, even that area had no palpable tenderness.
As I continued examining, I found a very eye-catching finding:
marked tenderness in the teres major.
The rest of the muscles and tendons were essentially negative.
The trap: a very convincing false lead
This kind of finding can easily mislead a clinician.
The teres major is one of the most common structures that produces pseudo-anterior shoulder pain. Although it lies posteriorly, tightness can alter humeral movement and project pain to the front of the shoulder.
Many clinicians — myself included — have been misled by the combination of:
Anterior shoulder pain + positive teres major tenderness
So at that moment, I treated it as a teres major dysfunction and performed needling and release.
The patient immediately felt “much lighter” and even said,
“Maybe I don’t need to come back.”
If the story ended there, it would look like a typical successful case — patient satisfied, symptoms improved.
But I was not satisfied.
The moment of doubt
What bothered me was the re-check.
After treatment:
-
External rotation still caused pain
-
Supine elevation still couldn’t reach the bed surface
In other words, symptoms improved slightly, but function did not truly recover.
Whenever I see this pattern, I have an internal rule:
The direction may be partially correct, but not deep enough.
Re-examination: digging one layer deeper
So I re-examined him more carefully and performed tests I hadn’t done initially.
I asked him to place his hand behind his back and gently pulled it outward.
This immediately triggered sharp anterior shoulder pain.
Then I asked him to push outward against resistance in the same position.
He had obvious weakness, again with anterior pain.
At that moment, it became clear in my mind:
Subscapularis.
The decisive test: axillary approach
To confirm, I performed a test I increasingly rely on —
axillary palpation.
Entering from the medial axilla and pressing along the anterior surface of the scapula toward the subscapularis, the result was unmistakable:
-
Severe tenderness
-
Pain radiating to the anterior shoulder
-
Perfect match with his chief complaint
At that point, the diagnosis was essentially confirmed.
The turning point in treatment
I immediately changed the treatment strategy.
Instead of focusing on compensatory structures, I performed:
-
Axillary subscapularis release
-
Deep finger separation technique
Initially, the patient experienced significant pain.
But as the tissue gradually softened, tolerance improved.
After the release, I reassessed immediately:
-
Supine elevation could now approach the bed surface
-
External rotation pain dropped markedly
-
Pain during overhead press and downward movement was greatly reduced
The patient felt the shoulder was “70–80% better.”
At that moment, he was relieved — and so was I.
Why this case is easy to miss
This case highlights three major pitfalls.
First, subscapularis injuries are often non-classical.
Superficial tenderness is minimal, and special tests are not always positive.
Second, the muscle lies too deep.
Without entering through the axillary route, the true lesion is often unreachable.
Third — and most important — compensatory deception.
When structures like the teres major or latissimus dorsi tighten, they can trap the clinician’s attention. You find a positive point, treat it, symptoms improve slightly, and you unconsciously believe you’ve found the cause.
That’s how diagnostic closure happens.
A deeper clinical lesson
This case reminded me of something important.
The most dangerous situation in clinical practice is not treatment failure —
it is partial success.
Because partial success makes you comfortable.
It makes you stop searching.
It prevents deeper thinking.
Many chronic shoulder cases become prolonged and recurrent for exactly this reason.
The real dividing line
Over the years, I’ve come to believe:
What truly separates clinicians is rarely technique.
It is depth of thinking.
Are you willing to admit that your first judgment might be incomplete?
Are you willing to step out of the compensatory layer
and search again for the real core?
That willingness is the true turning point in clinical growth.
 中文微信:nzacupunctureclinic
中文微信:nzacupunctureclinic
Leave a reply