Follow Dr. Win Huang to Learn Clinical Diagnosis (Case 9) A Long-Standing Digestive Disorder Improved Unexpectedly During Treatment for Low Back Pain
Follow Dr. Win Huang to Learn Clinical Diagnosis (Case 9)
A Long-Standing Digestive Disorder Improved Unexpectedly During Treatment for Low Back Pain
This is a very interesting clinical case.
The patient was an Indian man in his early forties. When he first came to see me, his main complaint was low back pain, which had troubled him for many years.
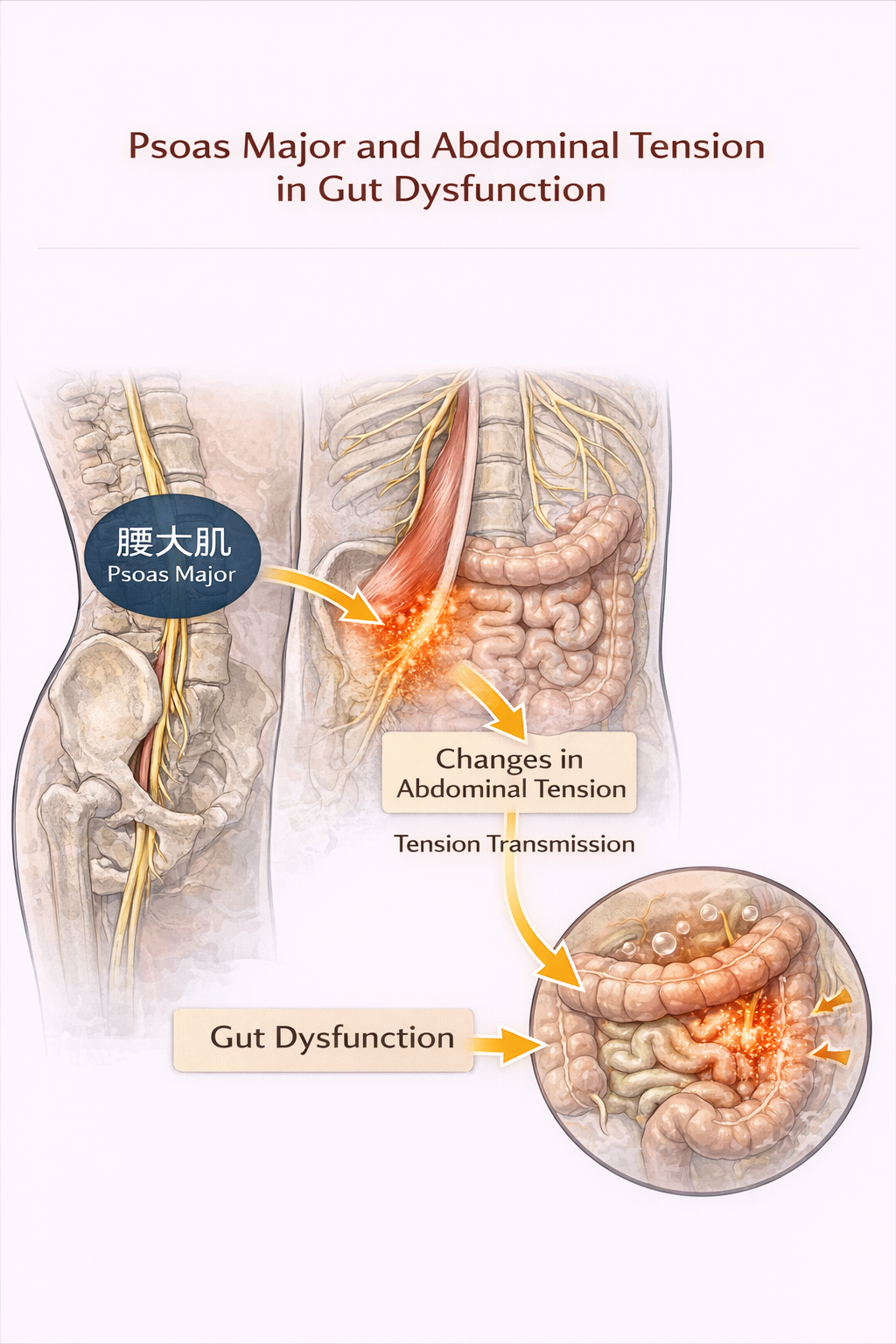
During the examination, I found that his psoas muscle was extremely tight. When I palpated the muscle through the abdomen, the tenderness was very strong and he could barely tolerate the pressure. If we use a pain scale of ten, the tenderness would be around eight or nine. The muscle also felt thick and tense on palpation, almost like a rope being pulled tight.
Therefore, in treating his low back pain, I focused mainly on releasing the psoas muscle. During each treatment session, I approached the muscle through the abdomen, located the most sensitive points, and used manual techniques to release the tension, combined with acupuncture therapy.
After about three treatments, his back pain improved significantly.
However, what happened next was quite unexpected.
At his third follow-up visit, the patient walked in looking very happy. He even wanted to give me a hug. He told me that his digestive system had changed dramatically over the past few days. The abdominal bloating that had troubled him for years had almost disappeared. His abdominal pain had also improved significantly. His abdomen felt softer, and bowel movements became much easier.
He also said that the strange feeling he used to have — as if his intestines were “stuck” or had stopped moving — was now gone.
Even more interesting, during the past few days he had tried eating some foods that he had previously avoided completely.
This change made him extremely happy because his digestive problems had bothered him for many years.
According to his description, his digestive issues had lasted for ten to twenty years, and had become much worse in recent years. He hardly dared to eat vegetables or fruit, because these foods would easily trigger bloating and abdominal pain. Therefore he had been very cautious with his diet.
He had consulted many specialists and had undergone numerous tests, including gastroscopy and abdominal ultrasound. However, no clear structural abnormalities were ever found. Doctors suggested that his condition might be related to gut microbiome imbalance or intestinal motility dysfunction.
He had even tried fecal microbiota transplantation in the hope of restoring healthy gut bacteria, but the results were limited.
So when his gastrointestinal symptoms suddenly improved, he was both surprised and delighted.
For me, the change was equally unexpected. My original intention had simply been to treat his back pain by releasing the psoas muscle tension. I had not anticipated that his digestive function would improve at the same time.
This made me begin to rethink an important question:
Could his long-standing digestive dysfunction be related to chronic tension of the psoas muscle?
During later examinations, I noticed that his abdomen had already become much softer and palpation produced almost no pain. However, the psoas muscle was still somewhat tight and enlarged, although less than before.
Therefore I decided to continue treating this area and observe whether further relaxation of the psoas muscle would continue to improve his digestive function and help maintain this improvement over time.
This case also led me to rethink a broader clinical question.
When facing gastrointestinal functional disorders, many acupuncture practitioners tend to explain them using broad concepts such as spleen-stomach imbalance, gut microbiota disturbance, or autonomic nervous system dysfunction.
These explanations are not necessarily wrong. The problem is that they are often too broad and too abstract.
When we stay only at this conceptual level, we may understand the theory, but in practical treatment we often lack a clear point of intervention.
However, if we shift our perspective slightly deeper and look at more specific structures — such as the fascia and muscles of the abdomen, deep muscles like the psoas, or the neural pathways around these structures — the situation may become very different.
Once we recognize that gastrointestinal dysfunction may be connected to these specific structures, we gain a concrete point of intervention in treatment. In other words, we finally have a place where we can truly apply our clinical skills.
When we only interpret disease through general concepts like spleen-stomach imbalance, microbiome disorder, or autonomic dysfunction, acupuncture practitioners often become merely participants in the treatment process.
But when we identify a specific structural level where intervention is possible, acupuncture practitioners have the opportunity to become the leading force in treating the condition.
Many so-called “functional disorders” may not be purely functional problems.
Sometimes we simply have not yet discovered their true structural entry point.
 中文微信:nzacupunctureclinic
中文微信:nzacupunctureclinic
Leave a reply