Follow Dr. Win Huang – Clinical Thinking Series 7 When a Locked Knee Is Not a Meniscus Tear
Follow Dr. Win Huang – Clinical Thinking Series 7
When a Locked Knee Is Not a Meniscus Tear
This case is a very typical example of how easily we can be misled by diagnostic labels.
The patient was a young man. Three months ago, he had been squatting at work for about five to ten minutes. The moment he stood up, he felt a sudden sharp pain in his left knee. The knee locked in flexion and he could not straighten it, so he went straight to the emergency department.
X-rays showed no obvious abnormality. The medical staff forcefully straightened the knee, but the pain remained and the movement was still restricted. He could not bend the knee properly. Anti-inflammatory painkillers helped a little during the day, but at night the pain became severe. No matter how he positioned the knee, he could not get comfortable and struggled to sleep.
After two weeks, the pain eased slightly, but the problem never truly resolved. The knee still had limited flexion and extension. He walked with a limp and needed a crutch. His GP suspected a meniscus injury and referred him to an orthopaedic specialist. He was still waiting for the appointment.
His mother is one of my long-term patients, so she suggested he come and see me.
Honestly, with a history like this, almost everyone would think of a meniscus tear first. Sudden pain after squatting, temporary locking, limited range — it all fits the textbook picture. But over the years, I’ve developed a habit: the more a case looks like the textbook, the more cautious I become.
On examination, the left knee showed clear restriction in flexion. He could only bend to a certain angle before pain stopped him, while the right heel could easily touch the buttock. In extension, the difference was also obvious. Lying supine, the right knee lay flat on the bed, but the left knee hovered above it. When I tried to push it straight, he felt the exact same pain — radiating from the medial knee down toward the inferior patella.
At this stage, I was still looking for evidence of a meniscus injury.
But the next step changed the direction of my thinking.
Joint line palpation was not very convincing. Meniscus provocation tests were not clearly positive. Instead, one very striking finding appeared: marked tenderness around the medial tibial condyle, and pressing this point reproduced pain radiating toward the lower patella. The moment I found this, I knew I had to change direction.
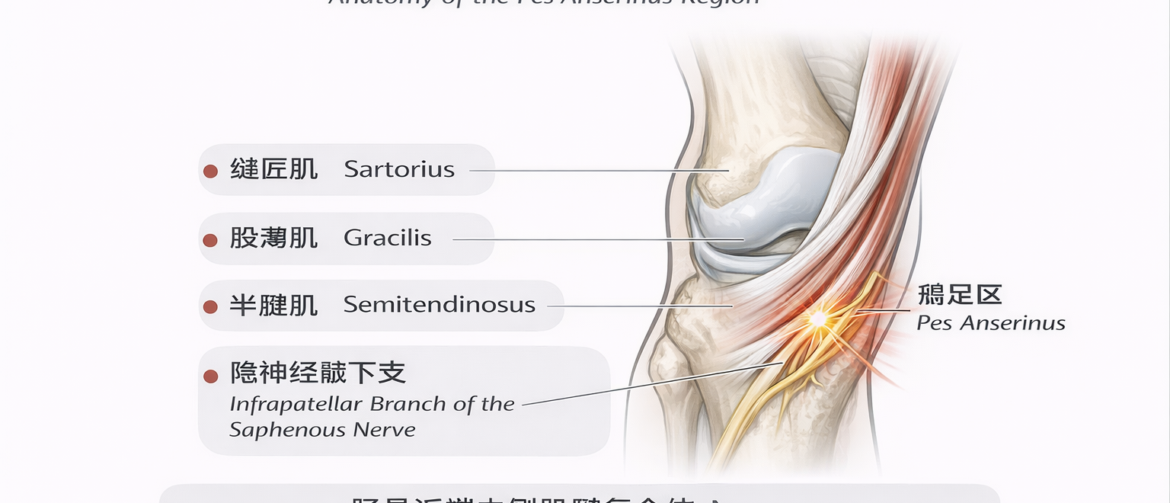
So I shifted my focus deeper into the soft tissue layer. That’s when I noticed several interesting findings. The sartorius was clearly tender. The semitendinosus and semimembranosus were also sensitive along the medial side. These muscles share one common insertion area — the proximal medial tibia, known clinically as the pes anserinus region.
At this point, the diagnostic layer had already shifted — from a joint problem to a soft-tissue corridor problem.
I went one step further and compared the medial knee sensation. The result was clear: the left medial knee was noticeably hypersensitive. Putting the clues together — pes anserinus tenderness, radiation toward the infrapatellar region, and local sensory change — one structure immediately came to mind: the infrapatellar branch of the saphenous nerve.
This structure is not unfamiliar in textbooks, but it is frequently overlooked in real clinical work. It runs right through the pes anserinus area. Once local fascial tension increases, it can easily become irritated and produce sharp, radiating pain.
Looking back at the original history, everything started to connect. Sudden pain after squatting does not always mean a meniscus tear. It can also result from sudden traction in the pes anserinus soft tissues, causing abrupt fascial tension changes and irritation of the saphenous nerve pathway.
Once the nerve is irritated, patients develop sharp pain and protective guarding. Clinically it may look like a locked knee, but in essence it is a functional lock rather than a mechanical one.
Once the thinking became clear, the treatment became simple.
Instead of focusing on the intra-articular structures, I directly addressed the soft-tissue corridor. I used localized bloodletting and cupping over the pes anserinus region to release medial fascial tension. After treatment, his pain dropped from about 7–8/10 to 3–4/10. His walking improved immediately, and he was able to walk without the crutch.
The most valuable part of this case is not the technique, but the thinking.
If I had followed the usual path, this would have remained a “possible meniscus tear” case — maybe temporary pain relief with acupuncture, then MRI, and eventually surgical discussions.
But once I shifted my perspective from structural labels to neural pathways, what looked complicated became clear. And the immediate treatment response became the strongest validation.
This case also carries a practical meaning for acupuncturists. When we can transform a “not treatable” meniscus label into a “treatable” soft-tissue condition, our role shifts — from participant to decision-maker.
Over the years, one realization has become clearer and clearer to me: many misjudgments do not happen because we lack knowledge, but because things look too familiar. Knee pain that looks like a meniscus tear, shoulder pain that looks like frozen shoulder, chronic pain that looks like arthritis — once a case is labelled as “typical,” our thinking easily becomes rigid.
Sometimes, when we look back, what truly locks the joint is not the structure itself, but our own thinking.
 中文微信:nzacupunctureclinic
中文微信:nzacupunctureclinic
Leave a reply