When Head Pain Is No Longer Just “Headache”
A Clinical Reflection on Sensory Hypersensitivity and System Amplification
A Patient Who Could Not Even Tolerate Touch
This patient was a woman in her sixties.
Three days before presentation, she suddenly developed severe pain over the left side of the head. Initially, the pain started around the top of the scalp, then gradually shifted toward the left temple region.
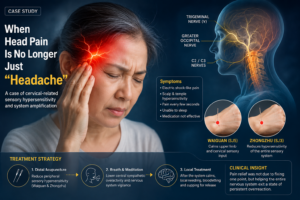
The pain was not dull or heavy like an ordinary headache. She described it as:
- electric shock-like
- stabbing
- pulsating
- intermittent
The attacks came every few seconds. Sometimes the interval was slightly longer, sometimes shorter.
But what stood out even more was the hypersensitivity.
The left scalp, temple area, and upper cervical region became extremely sensitive to touch. Even light contact over the skin aggravated the pain.
She could not sleep the entire night.
Pain medications, including carbamazepine and strong analgesics, provided little relief. She had also tried acupuncture elsewhere without significant improvement before attending my clinic.
Why This Did Not Behave Like a Simple Headache
At first glance, some clinicians might classify this as trigeminal neuralgia or severe migraine.
However, the overall clinical pattern suggested something more complex.
During examination, the most obvious finding was marked tenderness around the left C2–C3 cervical region. Compared with the right side, the upper cervical area was significantly more sensitive.
At the same time, the scalp itself had entered a highly reactive state.
This is important because:
the problem was no longer only about “where the pain was.”
The entire sensory system had become over-responsive.
When Multiple Sensory Systems Become Involved
In many chronic or severe pain cases, the issue is not simply one nerve being irritated.
Over time, multiple sensory systems may become involved together.
In this case, the upper cervical nerves, occipital nerves, trigeminal system, autonomic nervous system, emotional tension, and protective muscle guarding all appeared to participate together.
Eventually, the body entered a state of sensory amplification.
In this condition:
- normal touch becomes painful
- tension increases sensitivity
- anxiety increases pain intensity
- pain itself further drives nervous system reactivity
A self-reinforcing cycle develops.
This is why some patients gradually move beyond a simple “local nerve problem” into what is essentially a system-level hypersensitivity state.
Why I Did Not Start with Aggressive Local Treatment
At the beginning of treatment, I did not aggressively stimulate the painful scalp region.
Instead, I first used distal acupuncture points, including Waiguan (SJ5) and Zhongzhu (SJ3).
From my perspective, these points were not simply used to “reduce pain.”
Rather, the goal was to reduce the hypersensitive state within the upper limb, cervical, and head sensory pathways, allowing the peripheral sensory system to calm down first.
At the same time, I asked the patient to:
- slow her breathing
- close her eyes
- relax the body
- remain quiet
- focus on calming imagery and deep breathing
This was not merely psychological reassurance.
The purpose was to reduce the heightened central sympathetic activation and excessive nervous system vigilance.
Because many patients in this state enter a vicious cycle:
pain → tension → increased sensitivity → more pain
The nervous system remains trapped in a prolonged high-alert condition.
After about twenty to thirty minutes, the frequency and intensity of the attacks decreased significantly. The patient reported that the pain became much more tolerable.
Only after the system became calmer did I proceed with local treatment around the cervical region, including local bloodletting and cupping therapy.
Following treatment, the patient reported feeling noticeably lighter and more comfortable.
A Pattern I Have Seen Repeatedly
This was not the first time this patient experienced a similar episode.
About six months earlier, she had suffered a comparable attack that also improved after treatment and remained relatively stable for months.
This repeated pattern further supports the idea that some difficult pain conditions are not simply fixed structural lesions.
Instead, they may represent recurring episodes of sensory system sensitization involving multiple neural networks together.
Beyond “One Nerve, One Problem”
Many clinicians naturally try to identify a single structure:
- Which nerve?
- Which joint?
- Which exact point?
This type of thinking is important and necessary.
But in more complex chronic cases, the body often no longer behaves as a simple “single-point problem.”
Multiple systems may become involved simultaneously:
- sensory nerves
- autonomic nervous system
- emotional stress responses
- muscle guarding
- central amplification
At that stage, treatment also needs to move beyond purely local thinking.
Sometimes the goal is not simply to suppress pain.
Instead, the goal becomes:
helping the nervous system leave its prolonged high-alert state.
Clinical Insight
Many difficult pain conditions are not caused by a single damaged structure alone.
Over time, multiple systems may interact and reinforce each other, eventually creating a stable hypersensitive state within the nervous system.
In these situations, pain is no longer only about the original trigger.
The entire system has become involved.
This may explain why some patients continue to suffer despite normal imaging and why treatment aimed at only one local structure often fails.
Sometimes, pain improves not because one point has been “fixed,” but because the nervous system is no longer trapped in an ongoing state of overreaction.
Booking CTA
If you are experiencing ongoing nerve-related head pain, scalp sensitivity, or unexplained facial or cervical pain, you can book an appointment here:
 中文微信:nzacupunctureclinic
中文微信:nzacupunctureclinic
Leave a reply